
Sun Safety: Vitamin A to Zinc Oxide
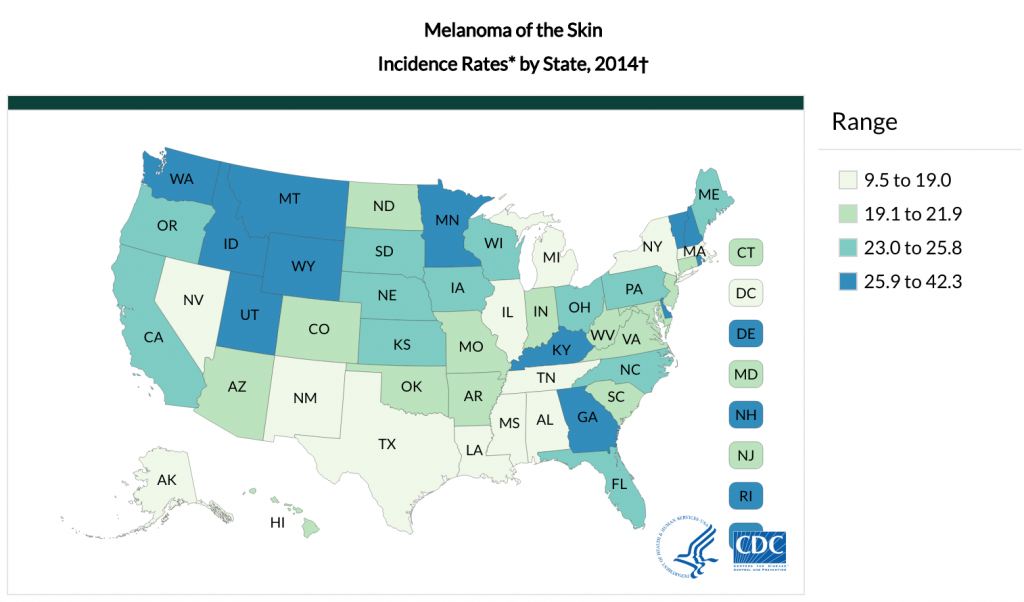
One in five Americans will get skin cancer in their lifetimes. The deadliest form, melanoma, is actually on the rise with an estimated 90,000 new cases in 2018. It might surprise you to hear it, but Washington has some of the highest rates for melanoma anywhere (4th in the U.S.)—and that includes the part of the state living near Puget Sound.
As the weather begins to transition and the sun shines through the clouds, you may begin to spend more time outdoors than you did this past winter. Of course, one of the most important parts to recreating outdoors is taking safety precautions from the elements. That’s why we asked UW Medicine skin expert Dr. Jennifer Gardner to share her insights about skin cancer prevention.
The following breaks down common sun- and sunscreen-related myths and misconceptions as well as provides updates about recent news and research developments. You can also view a Whole U seminar recording with Dr. Gardner discussing all of this and more!
Ultraviolet light is a known carcinogen.
The World Health Organization has declared ultraviolet (UV) light from the sun or from artificial sources such as tanning beds to be a known carcinogen—it causes cancer. Today, tanning beds are required to carry a Surgeon General’s warning that they will cause cancer. UVB rays (B for burning) are the ones that make the skin’s epidermis (outer layer of skin) red.
UVA rays penetrate deeper into a person’s second layer of skin—the dermis—and damage the structure-giving collagen in the skin, causing premature wrinkling and signs of aging. These rays are responsible for causing skin cancer, including the deadliest form of skin cancer, melanoma. Sun-protecting clothing and sunscreens either block or absorb these rays.
Don’t avoid the sun—just be smart about accumulation over time.
“You have to be smart, but you shouldn’t shy away from doing what you love,” says Gardner. “You just have to be smart and prepared about how you do it.” Everyday sun exposure does accumulate over time, she says, adding that the difference can be seen by comparing the top and underside of one’s arms. The more exposure you get, the higher your risk for skin cancers as you age.
“Frequent sunburn as a child or young adult does increase your risk for skin cancer,” Garner says. “Prevention is so much easier than treatment.”
There is no such thing as a “base tan.”
Intermittent sunburn is no joke. Occurring most frequently in instances of vacation or travel, “intermittent sun burn occurs when unprotected skin sees a lot of sun at once,” says Gardner. “Those are really bad for us, even if it’s just happening every year or so. That increases the risk for melanoma especially. There’s no such thing as a safe tan—tan on the skin is your cells’ way of telling you they are getting DNA damage from too much sun exposure.”
Tanning beds. Just don’t.
“We’re really learning this is not a good thing to do,” Gardner says.
Checking for melanoma is as easy as A-B-C-D-E.
- Asymmetrical spots should get checked.
- Border areas on skin that appear “scalloped” also beg getting checked.
- Color, often designated by darkening of skin cells or appearance of multiple colors, is another sign to get checked.
- Diameter indicates you should get checked when spots on the skin grow larger with time—anything larger than the size of a pencil eraser.
- Evolution. Pay attention to changes on your skin and get checked when one is observed.
PNW clouds do not make it safe.
“We live in a very deceptive part of the world,” Gardner says. “Sunscreen has to be a year-round commitment if you’re looking to avoid some of that exposure.” Snow, sand, water and high elevations are particular culprits when it comes to reflecting UV lights from all angles.
Sunglasses and shade are your friends.
“Sunglasses should be blocking UV light at 99-100%” Gardner says, also recommending taking care to apply sunscreen as close to one’s eyes as possible as skin cancer near one’s eyes is “not fun” to deal with as you age.
Another easy daily sun-protection ritual Gardner recommends is to find the shade and use it. Wearing sun-protective clothing is another of the surest ways to protect your body from the sun. Wide-brimmed hats go a long way when you’re on the move, says Gardner, who adds, “little decisions made over the course of a lifetime really matter.”
There’s no such thing as “waterproof” sunscreen.
Sunscreens are no longer permitted to print “water proof,” so instead now bear the labels “water-resistant” or “very water-resistant.” That allows you between 40-80 minutes to use the product before you need to reapply, Gardner says. The best bet? To reapply every couple hours.
Use an SPF of 30 or above.
SPF 30 absorbs 97% of UV light. “You may want to think about upping that [SPF] number if you are going to be going to an intensely sunny place,” Gardner says. A 1 oz “shot glass full” of sunscreen is the amount you want to use to cover most of your exposed areas.
Is sunscreen safe?
Yes. No matter what the internet might say, sunscreen won’t give you cancer based on current data. There is currently a legislative debate in Hawaii to prohibit the distribution of sunscreens containing the chemicals oxybenzone and octinoxate, spurred on by their possible impact on sea-dwelling organisms and coral reefs. In the future, there may be bans on how “nano” the nanoparticle sunscreens can get to be deemed “reef safe” but this isn’t currently on the table.
Vitamin D: eat it.
“Getting vitamin D through your skin is not very predictable, nor is it necessarily the best way to get it,” Gardner says. “If you’re being amazing at protecting yourself from the sun, you probably have low vitamin D.” The American Academy of Dermatology has issued the following position statement: “Adequate amount of vitamin D should be obtained from a healthy diet that includes foods naturally rich or fortified with vitamin D. [It] should not be obtained from unprotected exposure to ultraviolet radiation.”
Skin cancer prevention seminar
Get the full scoop by watching this seminar recording with Dr. Gardner! The Whole U was thrilled to host Dr. Gardner at the Husky Union Building in 2018 and looks forward to once again meeting in person when safe to do. For now, focus on your personal skin safety by tuning into this important recording.
 Jennifer M. Gardner, M.D. is an Assistant Professor in the Division of Dermatology at the University of Washington.
Jennifer M. Gardner, M.D. is an Assistant Professor in the Division of Dermatology at the University of Washington.
She specializes in pigmented lesions, melanoma, skin cancer, skin problems associated with chemotherapy or immunotherapies used to treat cancer, as well as general dermatology issues such as acne, psoriasis, atopic dermatitis, and infections of the skin.